by Diane Masson | Jul 26, 2015

Diane and her mom about a month before she died.
Let’s hear from professionals around the world to see if this assumption is correct! Do seniors need fewer days of hospice in assisted living and skilled nursing than at home? It makes sense to me.
An article by the Philly Voice stated, “At hospice enrollment, between 2008 and 2012, 78,130 of the patients in the study lived at home and 7,451 were in assisted living.”
My own mom with vascular dementia, living in skilled nursing care, only needed 4 days of hospice care. While my mom was actively dying with hospice care, I read about all the signs people show approaching death.
In a great little book called, “Gone from my Sight, The Dying Experience,” by Barbara Karnes, RN, I learned how seniors start to withdraw one to three months prior to death. The desire for food decreases while sleep dramatically increases. A senior can become more disoriented, agitated and talk with the unseen one or two weeks before death.
As I held my mom’s nonresponsive hand a few days before her death, I realized that most of what the book predicted had happened to my mom in the previous few months. Yet she was completely supported in her skilled nursing environment. What a gift that community gave her.
When she could not feed herself (she forgot how because of her dementia), the caregivers or I would feed her. At every meal she was given an opportunity to feed herself. The staff never gave up on her improving. If my mom had been home, I would have fretted and taken her to the doctor to learn why she was eating less.
My mom never had to be disrupted from her familiar environment and go the hospital like many hospice patients. All types of care could happen right at her skilled nursing community. My mom needed full care (bathing, dressing, medication management, two-person transfers, toileting and feeding).
I can see in my mind’s eye that many higher-level assisted livings could accomplish what my mom’s skilled nursing environment did for her. Calm caring 24/7 staff that understands declining seniors can bring a sense of peace to the patient and his or her family members.
I want to personally thank all the assisted living and skilled nursing care workers that help seniors transition to death. Bless you! Shout out to all the nurses and caregivers at Freedom Village Skilled Nursing for what you did for my mom. Your compassionate staff rocks!
Your Senior Housing Options,” has a simplistic title, but what’s inside this new book can save a you months of research time. Hear Diane Masson’s interview of how her mother and in-law’s faced the pivotal decision to plan ahead or wait until a crisis. Learn the pitfalls from transitioning from your home to senior housing. Understand what questions to ask, insider tips and dirty secrets revealed. The decision to stay home requires caregivers. Prevent elder abuse by determining if a home care agency is reputable, before they move into your home. You are just not looking for today’s needs, but for your future care. Discover key differences between rental facilities vs Continuing Care Retirement Communities. Do you have enough financial resources if you need to be in a higher level of care for an extended period of time? For weekly tips join at: Www.Tips2Seniors.com
Diane Masson has worked in senior housing for 17 years and is the regional marketing director for two debt-free Continuing Care Retirement Communities in Southern CA (Freedom Village in Lake Forest and The Village in Hemet). Her first book “Senior Housing Marketing – How to Increase Your Occupancy and Stay Full,” is being utilized by senior housing professionals across the country. Both her first book and second book, “Your Senior Housing Options,” have a 5-star rating on Amazon.com.

by Diane Masson | Apr 26, 2015

My Mom and I
My mother’s blood sugar spiked to 400 on Monday and 520 on Tuesday. She was fighting a UTI and ecoli. At 92, her body tried to fight it off. The doctor said the antibiotics would either work in two days or she would go down hill fast. It was the later.
The care ambassadors and nurses at Freedom Village were amazing. I lost count after twenty-three staff came in to say good-bye and provide loving care. One care ambassador said, “I’ve known your mom for two years and she was my family.” Another said, “Everyday she would greet me in the hall and compliment what I was wearing that day.” My favorite was someone reminding me of her love of cats and how she usually had one with her or would respond to the mechanical one that meowed, purred and moved. Her face would light up with joy.
My mom lived in a higher level of care for nine years. Seven years in assisted living and almost two years in skilled nursing in Lake Forest, CA. Six years ago, a doctor made a comment that her life was not worth living because she had dementia and couldn’t remember anything. I replied, “How many of your patients said thank you and complimented you today?” The doctor sheepishly said, “Only your mom.” I said, “Then she still is fulfilling her purpose isn’t she?” The doctor backed off and gave the best care until my mom left that Seattle hospital.
Through nine years of advocacy for my mom, I have done the best I was able, making decisions with the knowledge that I have. I am not a nurse and based my advocacy on her wishes and trying to keep her comfortable.
Extraordinary Versus Comfort Care
Hospice began on Tuesday and they were a Godsend. My husband was in Seattle saying goodbye to his dad on hospice when everything happened. A nurse, a social worker and a chaplain came from hospice to support my mom and me. I learned the differences between extraordinary care and comfort care at the end. The IV’s, antibiotics and unnecessary medicine disappeared. The morphine and adavan began.
Final Burst of Energy
After the chaplain said some beautiful words, my mom had what they call a “burst of energy.” I was holding her hand when she opened her eyes half way and said, “I love you,” seven times and “thank you” twice. Then she closed her eyes and the energy was gone. I will treasure that memory.
After she choked while attempting to eat, I said no more food. A caregiver patiently helped her drink some juice even though it took 15 minutes. That was the last time I saw her drink because she could not swallow again.
The turns every two hours caused her to cry out. The repositioning was to prevent bedsores. I called hospice when the gentle turns seemed to hurt her more and they said to reduce the turns to every three hours and give the morphine 20 minutes before. The nurses and care ambassadors were outstanding. This little tip made the gentle turns easier for her.
The last day, she started to moan with every exhale. I called hospice again. The gurgling in the throat had started and it was time to start the medication that helped with that. The director of nursing arrived before hospice and we started the PRN of morphine and adavan that had been preapproved by her wonderful doctor. Hospice increased the frequency of the medications to once an hour and said she was not to be turned again. Alleluia.
The director of nursing was there every hour to administer the comfort medications. I cannot say enough about the staff of Freedom Village Health Care Center and how they supported and loved my mom and I, to the end.
My husband came back from Seattle and the room filled with music. When the chaplain arrived they sang together and it felt like a send off party. Her doctor entered about this time, gave me a hug and said, “She is going out in style. I am so happy that she is comfortable.” A priest came to give her last rites. I said and prayed everything I wanted to with my mom and have zero regrets.
After nine hours, my husband and I decided to take a dinner break. The director of nursing said she would not leave my mother until we returned. Another change happened right before we got back.
The chaplain and hospice were called. The moan on each exhale came back and I requested more morphine for her. Her doctor gave permission. Chris and I sang a couple of songs to her. The chaplain arrived. I requested scripture and the chaplain was reading from the Gospel of John when she passed. God’s presence was in the room. She was comfortable and at peace.
Today is Sunday and I would normally go and visit with my mom. I wrote this blog to help me with my own grief today.
It seems ironic now, that my new book is dedicated to my mom. Writing this blog has been therapy for me over the last three years. After sharing numerous stories about my mom, several senior living people said you should write a book to help other seniors and their families. So I did and “Your Senior Housing Options” was published recently.
I love you mother and hope your stories in the book can help others learn their options and plan ahead. So many seniors wait until a crisis and lose their ability to choose like my in-laws did. The greatest gift my mom ever gave me was to plan ahead and move into a Continuing Care Retirement Community. Over 16 years, my mom had good transitions through three levels of care.

by Diane Masson | Apr 19, 2015
 If a senior living sales person or ANYONE said to you, “We are half sold out,” what would be your first thought? I bet, it would not create urgency for you to act now.
If a senior living sales person or ANYONE said to you, “We are half sold out,” what would be your first thought? I bet, it would not create urgency for you to act now.
When I was considering buying comedy tickets at the Improv last night, I inquired if the event was already sold out. The salesperson divulged, “We are half sold out. Getting tickets should be no problem. We are really surprised that only half the tickets have sold two days before the event.” I thought, oh, this comedian is not as popular as I thought. I will wait to buy my tickets. I was actually disappointed that the salesperson did not create urgency for a famous comic.
It was shocking to me that she would be so forth coming and I walked away disheartened. I told her that I would come back later and did. But I decided to not buy the tickets, because apparently I could just show up in a couple of days and buy the tickets on the day of the event. Her over sharing will continue to affect sales until a manager catches it.
The comedy club sales person over shared. What could she have said instead? “Gosh, let me check, I might be able to get you some tickets. It’s very unusual to have this comic coming to our location. How many tickets would you like?” I would have bought the tickets instantly.
Remember that famous Beanie Baby craze of the 1980’s? It was all about urgency for stuffed toys. Yes, I am the proud owner of 100 Ty bears and still like them.
What are your senior living sales people saying? Is your independent living, assisted living, or skilled nursing sales people saying, “I have quite a few rooms to choose from…”? Cough, cough… You will never fill up with this language. Everyone wants something that they can’t have. There is such a thing as divulging too much information. If a family is given the opportunity to put off the decision to move, they will. Ninety-six percent of seniors end up staying in their own home and not moving. Why encourage them to stay home? How about creating a solution for their needs and offering them the perfect apartment in your senior living community?
Every apartment is unique in some respect, such as the floor plan, the view or where it is situated in the building. Create value for every single senior living apartment. Teach urgency and watch your occupancy rise. I go into a lot more detail in my book, “Senior Housing Marketing – How to Increase Your Occupancy and Stay Full.”
Senior living communities have heavy attrition these days, so it can take two or three more move-ins than move-outs to move up one percent in occupancy. It’s always nice to see the arrow sliding up to 100% full.
So have you encountered too much honesty like me? Do you think it is stupid?
Everyone of us knows at least one senior that needs to move now. Here is a resource to help you or them make an informed decision. Diane Twohy Masson’s new guide book for seniors, “Your Senior Housing Options,” is available on Amazon.com with a 5-star rating. It reveals a proactive approach to navigating the complex maze of senior housing options. It will help you understand the costs and consequences of planning ahead or waiting too long. Learn firsthand tips from someone who is currently advocating for three aging parents.
Among the thousands of seniors she and her teams have assisted in finding the right senior living community, the most difficult case has been helping her own parent. Masson spent two years exploring senior housing options with her mother before finding the ideal Continuing Care Retirement Community for her. After eight years in this independent living setting, she helped her mother transition into an assisted living community. Seven years later, even as a senior housing expert, Masson struggled with the decision to move her mother into a skilled nursing community.
More related articles by Diane can be found at Tips2Seniors.com or like Tips 2 Seniors on Facebook.
Diane Twohy Masson has worked in senior housing since 1999. She is an award-winning certified aging services professional and the author of Senior Housing Marketing: How to Increase Your Occupancy and Stay Full for senior living professionals.

by Diane Masson | Feb 15, 2015

Bill and Amy in 2012
Aging parent’s decisions can drive us crazy or make us sick. When a parent with dementia stubbornly chooses to stay home, it can be heart breaking for the adult children. Watching a senior’s vitality fade is hard enough. But for an adult child to witness a parent’s poor hygiene, lack of nutrition by eating frozen dinners (not fresh food) and to see the absence of good judgment is tough and sad.
Some of us never get sick. Yet here I am, literally worried sick about my in-laws. A month ago my father-in-law, Bill, had a heart attack. My mother-in-law, Amy, with dementia was left alone for the majority of three days and nights as the local children rallied around the dad at the hospital. They did make sure she had food and medications. My husband and I hired a geriatric nurse to evaluate and help Amy. The nurse was to be our eyes and ears, since we live 1000 miles away. By the time the nurse intervened, Amy had become psychotic and had trouble recognizing her own children.
To make a long story short – my father-in-law never wanted to move to a retirement community or assisted living. He actually told my husband and I (working in the senior living business) that he understood that he would be waiting for a health crisis.
Well a crisis is one parent in the hospital and we had two. Over the last month, Bill improved enough to graduate from the hospital, to rehabilitating in skilled nursing care, to living permanently with his adult daughter in her home. He was told by professionals that he could no longer be Amy’s caregiver (he had been her caregiver for five years) and would need help for himself 24-hours a day. Pneumonia and a fall preceded the heart attack and now he has trouble catching his breath if he overexerts himself in any way and can’t remember to take his own medications because of dementia.
Let me fast forward on Amy’s simultaneous crisis. Amy’s Alzheimer’s prevented her from grasping that her husband of 65 years was in the hospital. She eloped (I think she walked away to search for her missing husband and ultimately the police found her) and hit a nurse in her confusion and anxious state. The police took her to the hospital and she resided in the emergency room for two days because they did not have a bed in the locked area. This is the part I don’t even want to imagine because I know they must have had to sedate her completely because she was an elopement risk.
A week later, both the skilled nursing community where Bill was getting rehab and the hospital where Amy resided wanted to discharge them simultaneously. The local children said that was impossible and they had to be discharged one at a time. So Bill was released first. Our goal was to have Amy placed in a quality secured memory care by the end of the next week. That week ended two days ago on Friday. Now it’s a holiday weekend and she is stuck in a locked psych ward in a hospital. Amy could have been discharged on Friday afternoon. The injustice of it all has made me sick. Next week I will share why Amy was not released – you will be shocked and disgusted.
Diane Masson’s new guide book for seniors, “Your Senior Housing Options,” will be will be coming soon to Amazon.com. If you sign up for my weekly newsletter on the right side of this blog, you will be notified when my new book becomes available. Check out my new website: Tips2Seniors.com or please follow me on Facebook.
Diane Twohy Masson is the author of “Senior Housing Marketing – How to Increase Your Occupancy and Stay Full,” available at Amazon.com with a 5-star rating. The book is required reading at George Mason University as a part of its marketing curriculum. Within this book, the author developed a sales & marketing method with 12 keys to help senior living providers increase their occupancy. Masson developed this expertise as a marketing consultant, sought-after blogger for senior housing and a regional marketing director of continuing care retirement communities in several markets. She has also been a corporate director of sales and a mystery shopper for independent living, assisted living, memory care and skilled care nursing communities in multiple states. Currently, Masson is setting move-in records as the regional marketing director of two debt-free Continuing Care Retirement Communities in Southern California – Freedom Village in Lake Forest and The Village in Hemet, California. Interestingly, this career started when she was looking for a place for her own mom and helped her loved one transition through three levels of care.
© Marketing 2 Seniors| Diane Twohy Masson 2015 All Rights Reserved. No part of this blog post may be reproduced, copied, modified or adapted, without the prior written consent of the author, unless otherwise indicated for stand-alone materials. You may share this website and or it’s content by any of the following means: 1. Using any of the share icons at the bottom of each page. 2. Providing a back-link or the URL of the content you wish to disseminate. 3. You may quote extracts from the website with attribution to Diane Masson CASP and link https://www.marketing2seniors.net For any other mode of sharing, please contact the author Diane Masson.
by Diane Masson | Dec 28, 2014
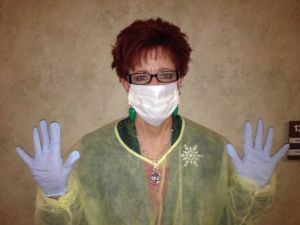
 What a sad circumstance for seniors to be alone during the holidays. Is the isolation voluntary or involuntary? My poor mom has ecoli and was put into isolation at her skilled nursing community. Everyone has to wear a gown, gloves and a mask to enter her room. She will NOT get to dine with her fellow residents for four more days. Fortunately, she is more than halfway through her antibiotic and feels good now. She was in great spirits today and even invited me to stay for lunch!
What a sad circumstance for seniors to be alone during the holidays. Is the isolation voluntary or involuntary? My poor mom has ecoli and was put into isolation at her skilled nursing community. Everyone has to wear a gown, gloves and a mask to enter her room. She will NOT get to dine with her fellow residents for four more days. Fortunately, she is more than halfway through her antibiotic and feels good now. She was in great spirits today and even invited me to stay for lunch!
Some seniors become isolated as they age in their home like my in-laws. They refuse to move to a retirement community. Both have dementia and neither of them drives. They are 100 percent dependent on one local son to bring them groceries, take them to the doctor and socialize with them. Is this enough human interaction? I don’t think so.
Other seniors determined to stay at home, use home care and become dependent on a single caregiver. Is this a healthy life? The rest of us interact with 10 or 20 people a day. What happens when someone only interacts with one person, day after day, month after month? Many years ago, my mom was in this situation and it was when the memory issues began.
Every senior faces a choice to plan ahead by moving to a senior living community or wait until a health care crisis and live with the consequences. I hope and pray that more seniors chose multiple human interactions by moving to a senior living community. My mom started to thrive again after she moved to assisted living. My in-laws could thrive again too, but they refuse.
My mom is in a good place and will see quite a few different staff during her isolation. My in-laws are 1000 miles away and will be in a lonely house for the holidays. The house can’t talk to them, smile at them or buy them groceries.
Diane Masson’s new guide book for seniors, “Your Senior Housing Options,” will be will be coming soon to Amazon.com. If you sign up for my weekly newsletter on the right side of this blog, you will be notified when my new book becomes available. Check out my new website: Tips2Seniors.com or please follow me on Facebook.
“Your Senior Housing Options,” is dedicated to my mother, whose stories are peppered throughout. Being her advocate for over ten years has taught me to be a better person. My mom has dementia, but I am truly blessed that she still calls me by name. Her smile and joy inspires me to see the positive side of life. It makes me want to reach out and help seniors and their families make better choices today so they can have more secure long-term care plans tomorrow.

by Diane Masson | Nov 2, 2014
 Am I a bad daughter? Yesterday, I learned the shocking truth that my mom has five missing teeth. My mom has lived in a higher level of care for over eight years. Seven years in assisted living in Seattle and the last 17 months in skilled nursing care in California.
Am I a bad daughter? Yesterday, I learned the shocking truth that my mom has five missing teeth. My mom has lived in a higher level of care for over eight years. Seven years in assisted living in Seattle and the last 17 months in skilled nursing care in California.
My mother has had vascular dementia for over 10 years and I have been attending doctor appointments with her for years. Why did I never consider oral health and attending a dentist appointment?
It was pure luck that I visited my mom this week when the mobile dentist was there. Dr. Mark Mroch was awesome. He had a funny and engaging personality. My mom was completely enamored with him. They were joking back and I forth and I was cracking up.
According to dental records the five teeth were missing when my mom arrived in California. Now that I have processed this situation, I have some unanswered dental questions:
- Why did no one tell the POA (Power of Attorney) of a dementia patient that her mom had five teeth missing when it was first discovered?
- Has my mom with her dementia been responsible for her own dental hygiene for all these years?
- Do assisted living and skilled nursing communities brush and floss teeth?
- How often?
- If the senior tells the caregiver that flossing hurts, do they just discontinue flossing and not tell the family?
- Is a dentist required to request flossing in order for it to happen?
Can you please share what the oral hygiene policy is at your assisted living, skilled nursing or memory care community? I know the goal is to have the residents be as independent as possible and brush his or her own teeth. What if they are not doing a good job? When does staff step in to help? Do staff actually watch them brush their teeth or is this one of those back burner items that can get overlooked?
My mom lived in a social model of assisted living. She was borderline skilled nursing for a year or so before we moved her. Is the dental program for dementia different in a social vs. medical model of assisted living?
Please help me figure this out and maybe we can help some POA’s out there who never thought about oral hygiene before. It’s vital that we advocate for our loved one.
Thanks, Diane
Diane Twohy Masson writes this weekly blog to support and engage with other senior housing professionals. Her first book is Senior Housing Marketing – How To Increase Your Occupancy and Stay Full. Many sales teams and organizations have used the 12 keys contained in this book for their weekly book review.
Diane Masson has recently created a New Guide for the Silver Tsunami. Her second book offers a pro-active approach for a senior to navigate his or her way through the senior housing market. “Selecting Senior Housing Options for Seniors IN the Silver Tsunami” is coming soon to Amazon.com. www.tips2seniors.com
© Marketing 2 Seniors| Diane Twohy Masson 2014 All Rights Reserved. No part of this blog post may be reproduced, copied, modified or adapted, without the prior written consent of the author, unless otherwise indicated for stand-alone materials. You may share this website and or it’s content by any of the following means: 1. Using any of the share icons at the bottom of each page. 2. Providing a back-link or the URL of the content you wish to disseminate. 3. You may quote extracts from the website with attribution to Diane Masson CASP and link https://www.marketing2seniors.net For any other mode of sharing, please contact the author Diane Masson.